Abstract
Objective
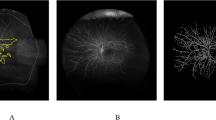
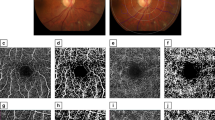
To present a fluorescein angiography (FA)‒based computer algorithm for quantifying retinal blood flow, perfusion, and permeability, in patients with diabetic retinopathy (DR). Secondary objectives were to quantitatively assess treatment efficacy following panretinal photocoagulation (PRP) and define thresholds for pathology based on a new retinovascular function (RVF) score for quantifying disease severity.
Methods
FA images of 65 subjects (58 patients and 7 healthy volunteers) were included. Dye intensity kinetics were derived using pixel-wise linear regression as a measure of retinal blood flow, perfusion, and permeability. Maps corresponding to each measure were then generated for each subject and segmented further using an ETDRS grid. Non-parametric statistical analyses were performed between all ETDRS subfields. For 16 patients, the effect of PRP was measured using the same parameters, and an amalgam of RVF was used to create an RVF index. For ten post-treatment patients, the change in FA-derived data was compared to the macular thickness measured using optical coherence tomography.
Results
Compared to healthy controls, patients had significantly lower retinal and regional perfusion and flow, as well as higher retinal permeability (p < 0.05). Moreover, retinal flow was inversely correlated with permeability (R = –0.41; p < 0.0001). PRP significantly reduced retinal permeability (p < 0.05). The earliest marker of DR was reduced retinal blood flow, followed by increased permeability. FA-based RVF index was a more sensitive indicator of treatment efficacy than macular thickness.
Conclusions
Our algorithm can be used to quantify retinovascular function, providing an earlier diagnosis and an objective characterisation of disease state, disease progression, and response to treatment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Flocks M, Miller J, Chao P. Retinal circulation time with the aid of fundus cinephotography. Am J Ophthalmol. 1959;48:3–10.
Friedman SM, Margo CE. Choroidal neovascular membranes: reproducibility of angiographic interpretation. Am J Ophthalmol. 2000;130:839–41.
Bertram B, Wolf S, Fiehöfer S, Schulte K, Arend O, Reim M. Retinal circulation times in diabetes mellitus type 1. Br J Ophthalmol. 1991;75:462–5.
Tomic L, Mäepea O, Sperber GO, Alm A. Comparison of retinal transit times and retinal blood flow: a study in monkeys. Invest Ophthalmol Vis Sci. 2001;42:752–5.
Or C, Sabrosa AS, Sorour O, Arya M, Waheed N. Use of OCTA, FA, and ultra-widefield imaging in quantifying retinal ischemia: a review. Asia-Pac J Ophthalmol. 2018;7:46–51.
Tan CS, Li KZ, Sadda SR. Wide-field angiography in retinal vein occlusions. Int J Retin Vitreous. 2019;5:18.
Fan W, Uji A, Wang K, Falavarjani KG, Wykoff CC, Brown DM, et al. Severity of diabetic macular edema correlates with retinal vascular bed area on ultra-wide field fluorescein angiography: DAVE study. Retina. 2000;40:1029–37.
Yu G, Aaberg MT, Patel TP, Iyengar RS, Powell C, Tran A, et al. Quantification of retinal nonperfusion and neovascularization with ultrawidefield fluorescein angiography in patients with diabetes and associated characteristics of advanced disease. JAMA Ophthalmol. 2020;138:680–8.
Tan CS, Chew MC, van Hemert J, Singer MA, Bell D, Sadda SR. Measuring the precise area of peripheral retinal non-perfusion using ultra-widefield imaging and its correlation with the ischaemic index. Br J Ophthalmol. 2016;100:235–9.
Serlin Y, Tal G, Chassidim Y, Parmet Y, Tomkins O, Knyazer B, et al. Novel fluorescein angiography-based computer-aided algorithm for assessment of retinal vessel permeability. PLoS One. 2013;8:e61599.
Prager O, Chassidim Y, Klein C, Levi H, Shelef I, Friedman A. Dynamic in vivo imaging of cerebral blood flow and blood-brain barrier permeability. Neuroimage. 2010;49:337–44.
Rublee E, Rabaud V, Konolige K, Bradski G. ORB: an efficient alternative to SIFT or SURF. Abstracts of the 2011 International Conference on Computer Vision. Barcelona, Spain: 2011. p. 2564–71.
Early Treatment Diabetic Retinopathy Study Research Group. Classification of diabetic retinopathy from fluorescein angiograms. Ophthalmology. 1991;98:807–22.
Schoknecht K, Prager O, Vazana U, Kamintsky L, Harhausen D, Zille M, et al. Monitoring stroke progression: In vivo imaging of cortical perfusion, blood-brain barrier permeability and cellular damage in the rat photothrombosis model. J Cereb Blood Flow Metab. 2014;34:1791–801.
Yu Y, Han Q, Ding X, Chen Q, Ye K, Zhang S, et al. Defining core and penumbra in ischemic stroke: a voxel- and volume-based analysis of whole brain CT perfusion. Sci Rep. 2006;6:1–7.
Bivard A, Levi C, Krishnamurthy V, Hislop-Jambrich J, Salazar P, Jackson B, et al. Defining acute ischemic stroke tissue pathophysiology with whole brain CT perfusion. J Neuroradiol. 2014;41:307–15.
Brown JC, Solomon SD, Bressler SB, Schachat AP, DiBernardo C, Bressler NM. Detection of diabetic foveal edema: contact lens biomicroscopy compared with optical coherence tomography. Arch Ophthalmol. 2004;122:330–5.
Levin AM, Rusu I, Orlin A, Gupta MP, Coombs P, D’Amico DJ, et al. Retinal reperfusion in diabetic retinopathy following treatment with anti-VEGF intravitreal injections. Clin Ophthalmol. 2017;11:193–200.
Pournaras CJ, Riva CE. Retinal blood flow evaluation. Ophthalmologica. 2013;229:61–74.
Aiello LP. Angiogenic pathways in diabetic retinopathy. N Engl J Med. 2005;353:839–41.
Couturier A, Rey P-A, Erginay A, Lavia C, Bonnin S, Dupas B, et al. Widefield OCT-angiography and fluorescein angiography assessments of nonperfusion in diabetic retinopathy and edema treated with anti-vascular endothelial growth factor. Ophthalmology. 2019;126:1685–94.
Jampol LM, Glassman AR, Sun J. Evaluation and care of patients with diabetic retinopathy. N Engl J Med. 2020;382:1629–37.
Jia Y, Bailey ST, Hwang TS, McClintic SM, Gao SS, Pennesi ME, et al. Quantitative optical coherence tomography angiography of vascular abnormalities in the living human eye. Proc Natl Acad Sci USA. 2015;112:E2395–402.
Wessel MM, Aaker GD, Parlitsis G, Cho M, D’Amico DJ, Kiss S. Ultra-wide-field angiography improves the detection and classification of diabetic retinopathy. Retina. 2012;32:785–91.
Silva PS, Cavallerano JD, Haddad NMN, Kwak H, Dyer KH, Omar AF, et al. Peripheral lesions identified on ultrawide field imaging predict increased risk of diabetic retinopathy progression over 4 years. Ophthalmology. 2015;122:949–56.
Talks SJ, Manjunath V, Steel DHW, Peto T, Taylor R. New vessels detected on widefield imaging compared to twofield and sevenfield imaging: Implications for diabetic retinopathy screening image analysis. Br J Ophthalmol. 2015;99:1606–9.
Aiello LP, Odia I, Glassman AR, Melia M, Jampol LM, Bressler NM, et al. Comparison of Early Treatment Diabetic Retinopathy Study standard 7-field imaging with ultrawide-field imaging for determining severity of diabetic retinopathy. JAMA Ophthalmol. 2019;137:65–73.
Grunwald JE, Riva CE, Sinclair SH, Brucker AJ, Petrig BL. Laser doppler velocimetry study of retinal circulation in diabetes mellitus. Arch Ophthalmol. 1986;104:991–6.
Grunwald JE, Brucker AJ, Petrig BL, Riva CE. Retinal blood flow regulation and the clinical response to panretinal photocoagulation in proliferative diabetic retinopathy. Ophthalmology. 1989;96:1518–22.
Grunwald JE, Brucker AJ, Grunwald SE, Riva CE. Retinal hemodynamics in proliferative diabetic retinopathy. A laser doppler velocimetry study. Invest Ophthalmol Vis Sci. 1993;34:66–71.
Russell JF, Al-Khersan H, Shi Y, Scott NL, Hinkle JW, Fan KC, et al. Retinal nonperfusion in proliferative diabetic retinopathy before and after panretinal photocoagulation assessed by widefield OCT angiography. Am J Ophthalmol. 2020;213:177–85.
Wykoff CC, Shah C, Dhoot D, Coleman HR, Thompson D, Du W, et al. Longitudinal retinal perfusion status in eyes with diabetic macular edema receiving intravitreal aflibercept or laser in VISTA study. Ophthalmology. 2019;126:1171–80.
Bressler NM, Beck RW, Ferris FL. Panretinal photocoagulation for proliferative diabetic retinopathy. N Engl J Med. 2011;365:1520–6.
Tan B, Chua J, Lin E, Cheng J, Gan A, Yao X, et al. Quantitative microvascular analysis with wide-field optical coherence tomography angiography in eyes with diabetic retinopathy. JAMA Netw Open. 2020;3:1–13.
Lujan BJ, Calhoun CT, Glassman AR, Googe JM, Jampol LM, Melia M, et al. Optical coherence tomography angiography quality across three multicenter clinical studies of diabetic retinopathy. Transl Vis Sci Technol. 2021;10:1–10.
Author information
Authors and Affiliations
Contributions
The authors’ responsibilities were as follows: AF and JL formulated the research question and designed the study; AW, AC, YS and JL obtained data; AA analysed the data; AA, OT-N, AL, YS and JL: interpreted the findings and wrote the article. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
AA and AF: Emagix, Inc., Halifax, Nova Scotia, Canada. The other authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Abbasnejad, A., Tomkins-Netzer, O., Winter, A. et al. A fluorescein angiography-based computer-aided algorithm for assessing the retinal vasculature in diabetic retinopathy. Eye 37, 1293–1301 (2023). https://doi.org/10.1038/s41433-022-02120-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-022-02120-4