Abstract
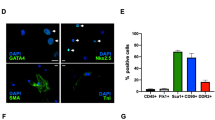
Cell-based therapy using adipose-derived stem cells (ADSCs) has emerged as a novel therapeutic approach to treat heart failure after myocardial infarction (MI). The purpose of this study was to determine whether inhibition of α1-adrenergic receptors (α1-ARs) in ADSCs attenuates ADSC sheet-induced improvements in cardiac functions and inhibition of remodeling after MI. ADSCs were isolated from fat tissues of Lewis rats. In in vitro studies using cultured ADSCs, we determined the mRNA levels of vascular endothelial growth factor (VEGF)-A and α1-AR under normoxia or hypoxia and the effects of norepinephrine and an α1-blocker, doxazosin, on the mRNA levels of angiogenic factors. Hypoxia increased α1-AR and VEGF mRNA levels in ADSCs. Norepinephrine further increased VEGF mRNA expression under hypoxia; this effect was abolished by doxazosin. Tube formation of human umbilical vein endothelial cells was promoted by conditioned media of ADSCs treated with the α1 stimulant phenylephrine under hypoxia but not by those of ADSCs pretreated with phenylephrine plus doxazosin. In in vivo studies using rats with MI, transplanted ADSC sheets improved cardiac functions, facilitated neovascularization, and suppressed fibrosis after MI. These effects were abolished by doxazosin treatment. Pathway analysis from RNA sequencing data predicted significant upregulation of α1-AR mRNA expression in transplanted ADSC sheets and the involvement of α1-ARs in angiogenesis through VEGF. In conclusion, doxazosin abolished the beneficial effects of ADSC sheets on rat MI hearts as well as the enhancing effect of norepinephrine on VEGF expression in ADSCs, indicating that ADSC sheets promote angiogenesis and prevent cardiac dysfunction and remodeling after MI via their α1-ARs.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Hirche H, Franz C, Bös L, Bissig R, Lang R, Schramm M. Myocardial extracellular K+ and H+ increase and noradrenaline release as possible cause of early arrhythmias following acute coronary artery occlusion in pigs. J Mol Cell Cardiol. 1980;12:579–93.
Kurz T, Yamada KA, DaTorre SD, Corr PB. Alpha 1–adrenergic system and arrhythmias in ischaemic heart disease. Eur Heart J. 1991;12:88–98.
Gregorini L, Marco J, Palombo C, Kozàkovà M, Anguissola GB, Cassagneau B, et al. Postischemic left ventricular dysfunction is abolished by alpha-adrenergic blocking agents. J Am Coll Cardiol. 1998;31:992–1001.
Gregorini L, Fajadet J, Robert G, Cassagneau B, Bernis M, Marco J. Coronary vasoconstriction after percutaneous transluminal coronary angioplasty is attenuated by antiadrenergic agents. Circulation. 1994;90:895–907.
Yamamoto K, Kurata Y, Inoue Y, Adachi M, Tsuneto M, Miake J, et al. Pretreatment with an angiotensin II receptor blocker abolished ameliorating actions of adipose-derived stem cell sheets on cardiac dysfunction and remodeling after myocardial infarction. Regen Ther. 2018;9:79–88.
Jiang Q, Ding S, Wu J, Liu X, Wu Z. Norepinephrine stimulates mobilization of endothelial progenitor cells after limb ischemia. PLoS ONE. 2014;9:e101774. https://doi.org/10.1371/journal.pone.0101774.
Wu B, Wang L, Yang X, Mao M, Ye C, Liu P, et al. Norepinephrine inhibits mesenchymal stem cell chemotaxis migration by increasing stromal cell-derived factor-1 secretion by vascular endothelial cells via NE/abrd3/JNK pathway. Exp Cell Res. 2016;349:214–20. https://doi.org/10.1016/j.yexcr.2016.09.007.
Candipan RC, Hsiun PT, Pratt R, Cooke JP. Vascular injury augments adrenergic neurotransmission. Circulation. 1994;89:777–84.
Chalothorn D, Zhang H, Clayton JA, Thomas SA, Faber A. Catecholamine augments collateral vessel growth and angiogenesis in hindlimb ischemia. Am J Physiol Heart Circ Physiol. 2005;289:H947–59.
Vinci MC, Bellik L, Filippi S, Ledda F, Parenti A. Trophic effects induced by alpha1D-adrenoceptors on endothelial cells are potentiated by hypoxia. Am J Physiol Heart Circ Physiol. 2007;293:H2140–7.
Kawamura M, Miyagawa S, Miki K, Saito A, Fukushima S, Higuchi T, et al. Feasibility, safety, and therapeutic efficacy of human induced pluripotent stem cell-derived cardiomyocyte sheets in a porcine ischemic cardiomyopathy model. Circulation. 2012;126:S29–37.
Menasché P, Alfieri O, Janssens S, McKenna W, Reichenspurner H, Trinquart L, et al. The myoblast autologous grafting in ischemic cardiomyopathy (MAGIC) trial: first randomized placebo-controlled study of myoblast transplantation. Circulation. 2008;117:1189–200.
Bolli R, Tang XL, Sanganalmath SK, Rimoldi O, Mosna F, Abdel-Latif A, et al. Intracoronary delivery of autologous cardiac stem cells improves cardiac function in a porcine model of chronic ischemic cardiomyopathy. Circulation. 2013;128:122–31.
Zhao T, Zhao W, Meng W, Liu C, Chen Y, Gerling IC, et al. VEGF-C/VEGFR-3 pathway promotes myocyte hypertrophy and survival in the infarcted myocardium. Am J Transl Res. 2015;7:697–709.
Rong SL, Wang XL, Zhang CY, Song ZH, Cui LH, He XF, et al. Transplantation of HGF gene-engineered skeletal myoblasts improve infarction recovery in a rat myocardial ischemia model. PLoS ONE. 2017;12:e0175807. https://doi.org/10.1371/journal.pone.0175807.
Liu J, Wu P, Wang Y, Du Y, Nan A, Liu S, et al. Ad-HGF improves the cardiac remodeling of rat following myocardial infarction by upregulating autophagy and necroptosis and inhibiting apoptosis. Am J Transl Res. 2016;8:4605–27.
Terajima Y, Shimizu T, Tsuruyama S, Sekine H, Ishii H, Yamazaki K, et al. Autologous skeletal myoblast sheet therapy for porcine myocardial infarction without increasing risk of arrhythmia. Cell Med. 2013;6:99–109.
Song H, Cha MJ, Song BW, Kim IK, Chang W, Lim S, et al. Reactive oxygen species inhibit adhesion of mesenchymal stem cells implanted into ischemic myocardium via interference of focal adhesion complex. Stem Cells. 2010;28:555–63.
Hamdi H, Planat-Benard V, Bel A, Puymirat E, Geha R, Pidial L, et al. Epicardial adipose stem cell sheets results in greater post-infarction survival than intramyocardial injections. Cardiovasc Res. 2011;91:483–91.
Patila T, Miyagawa S, Imanishi Y, Fukushima S, Siltanen A, Mervaala E, et al. Comparison of arrhythmogenicity and proinflammatory activity induced by intramyocardial or epicardial myoblast sheet delivery in a rat model of ischemic heart failure. PLoS ONE. 2015;10:e0123963. https://doi.org/10.1371/journal.pone.0123963.
Memon IA, Sawa Y, Fukushima N, Matsumiya G, Miyagawa S, Taketani S, et al. Repair of impaired myocardium by means of implantation of engineered autologous myoblast sheets. J Thorac Cardiovasc Surg. 2005;130:1333–41.
Sekiya N, Matsumiya G, Miyagawa S, Saito A, Shimizu T, Okano T, et al. Layered implantation of myoblast sheets attenuates adverse cardiac remodeling of the infarcted heart. J Thorac Cardiovasc Surg. 2009;138:985–93.
Gnecchi M, Zhang Z, Ni A, Dzau VJ. Paracrine mechanisms in adult stem cell signaling and therapy. Circ Res. 2008;103:1204–19.
Harada Y, Yamamoto Y, Tsujimoto S, Matsugami H, Yoshida A, Hisatome I. Transplantation of freshly isolated adipose tissue-derived regenerative cells enhances angiogenesis in a murine model of hind limb ischemia. Biomed Res. 2013;34:23–9.
Miranville A, Heeschen C, Sengenès C, Curat CA, Busse R, Bouloumié A. Improvement of postnatal neovascularization by human adipose tissue-derived stem cells. Circulation. 2004;110:349–55.
Nakagami H, Maeda K, Morishita R, Iguchi S, Nishikawa T, Takami Y, et al. Novel autologous cell therapy in ischemic limb disease through growth factor secretion by cultured adipose tissue-derived stromal cells. Arterioscler Thromb Vasc Biol. 2005;25:2542–47.
Rehman J, Traktuev D, Li J, Merfeld-Clauss S, Temm-Grove CJ, Bovenkerk JE, et al. Secretion of angiogenic and antiapoptotic factors by human adipose stromal cells. Circulation. 2004;109:1292–8.
Otsuki Y, Nakamura Y, Harada S, Yamamoto Y, Ogino K, Morikawa K, et al. Adipose stem cell sheets improved cardiac function in the rat myocardial infarction, but did not alter cardiac contractile responses to β-adrenergic stimulation. Biomed Res. 2015;36:11–9.
Shannon R, Chaudhry M. Effect of alpha1-adrenergic receptors in cardiac pathophysiology. Am Heart J. 2006;152:842–50.
Adachi M, Watanabe M, Kurata Y, Inoue Y, Notsu T, Yamamoto K, et al. β-Adrenergic blocker, carvedilol, abolishes ameliorating actions of adipose-derived stem cell sheets on cardiac dysfunction and remodeling after myocardial infarction. Circ J. 2019;83:2282–91.
Watanabe M, Horie H, Kurata Y, Inoue Y, Notsu T, Wakimizu T, et al. Esm1 and Stc1 as angiogenic factors responsible for protective actions of adipose-derived stem cell sheets on chronic heart failure after rat myocardial infarction. Circ J. 2021;85:657–66.
Shibata R, Murohara T. Future of therapeutic angiogenesis using adipose-derived stem cells in the cardiovascular field. Circ J. 2021;85:667–8.
Simons M, Gordon E, Claesson-Welsh L. Mechanisms and regulation of endothelial VEGF receptor signalling. Nat Rev Mol Cell Biol. 2016;17:611–25.
Eckhart AD, Yang N, Xin X, Faber JE. Characterization of the alpha1B-adrenergic receptor gene promoter region and hypoxia regulatory elements in vascular smooth muscle. Proc Natl Acad Sci USA. 1997;94:9487–92.
Semenza GL. Transcriptional regulation by hypoxia-inducible factor 1 molecular mechanisms of oxygen homeostasis. Trends Cardiovasc Med. 1996;6:151–7.
Lutgendorf SK, Cole S, Costanzo E, Bradley S, Coffin J, Jabbari S, et al. Stress-related mediators stimulate vascular endothelial growth factor secretion by two ovarian cancer cell lines. Clin Cancer Res. 2003;9:4514–21.
Teeters JC, Erami C, Zhang H, Faber JE. Systemic α1A-adrenoceptor antagonist inhibits neointimal growth after balloon injury of rat carotid artery. Am J Physiol Heart Circ Physiol. 2003;284:H385–92.
Ciccarelli M, Santulli G, Campanile A, Galasso G, Cervèro P, Altobelli GG, et al. Endothelial alpha1-adrenoceptors regulate neo-angiogenesis. Br J Pharmacol. 2008;153:936–46.
Pan SL, Guh JH, Huang YW, Chern JW, Chou JY, Teng CM. Identification of apoptotic and antiangiogenic activities of terazosin in human prostate cancer and endothelial cells. J Urol. 2003;169:724–9.
Keledjian K, Garrison JB, Kyprianou N. Doxazosin inhibits human vascular endothelial cell adhesion, migration, and invasion. J Cell Biochem. 2005;94:374–88.
Liao C-H, Guh J-H, Chueh S-C, Yu H-J. Anti-angiogenic effects and mechanism of prazosin. Prostate. 2011;71:976–84.
Mortensen SP, Egginton S, Madsen M, Hansen JB, Munch GDW, Iepsen UW, et al. Alpha adrenergic receptor blockade increases capillarization and fractional O2 extraction and lowers blood flow in contracting human skeletal muscle. Acta Physiol. 2017;221:32–43.
Tyurin-Kuzmin PA, Fadeeva JI, Kanareikina MA, Kalinina NI, Sysoeva VY, Dyikanov DT, et al. Activation of β-adrenergic receptors is required for elevated α1A-adrenoreceptors expression and signaling in mesenchymal stromal cells. Sci Rep. 2016;6:32835. https://doi.org/10.1038/srep32835.
Shionoiri H, Yasuda G, Yoshimura H, Umemura S, Miyajima E, Miyakawa T, et al. Antihypertensive effects and pharmacokinetics of single and consecutive administration of doxazosin in patients with mild to moderate essential hypertension. Cardiovasc Pharmacol. 1987;10:90–5.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
IH reported receiving lecturer’s fee from Mochida Pharmaceutical Company; Sanwa Kagaku Kenkyusho Co., Ltd.; Teijin Pharma Co., Ltd.; and Fuji Yakuhin Co., Ltd., and research grants from Mochida Pharmaceutical Company; Teijin Pharma; Fuji Yakuhin Co., Ltd.; and Sanwa Kagaku Kenkyusho Co., Ltd.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Horie, H., Hisatome, I., Kurata, Y. et al. α1-Adrenergic receptor mediates adipose-derived stem cell sheet-induced protection against chronic heart failure after myocardial infarction in rats. Hypertens Res 45, 283–291 (2022). https://doi.org/10.1038/s41440-021-00802-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-021-00802-2
Keywords
This article is cited by
-
Effects of miR126 Expressing Adipose-Derived Stem Cells on Fat Graft Survival and Angiogenesis
Aesthetic Plastic Surgery (2023)