A Minnesota man with COVID-19 and severe gastrointestinal bleeding died recently after waiting days for an intensive care unit (ICU) bed, the Associated Press reported.
When a hospital ran out of blood for 87-year-old Bob Cameron, state troopers drove 130 miles to deliver blood for him. Cameron, who had checked into his hometown hospital in Hallock, waited two days to get into an ICU, the AP reported. The troopers shuttled blood to the hospital all the way from Fargo, North Dakota, to keep him alive while officials searched for an opening in a larger facility.
Cameron was finally given a bed on October 12 at Sanford Health in Fargo, but after he had an operation there his condition worsened and he died October 13, the Star Tribune in Minneapolis reported.
"We can't say for certain, of course, that if he got to an ICU bed sooner that he would have survived, but we just feel in our hearts that he would have," said Cameron's granddaughter, Janna Curry.
For more reporting from the Associated Press, see below.
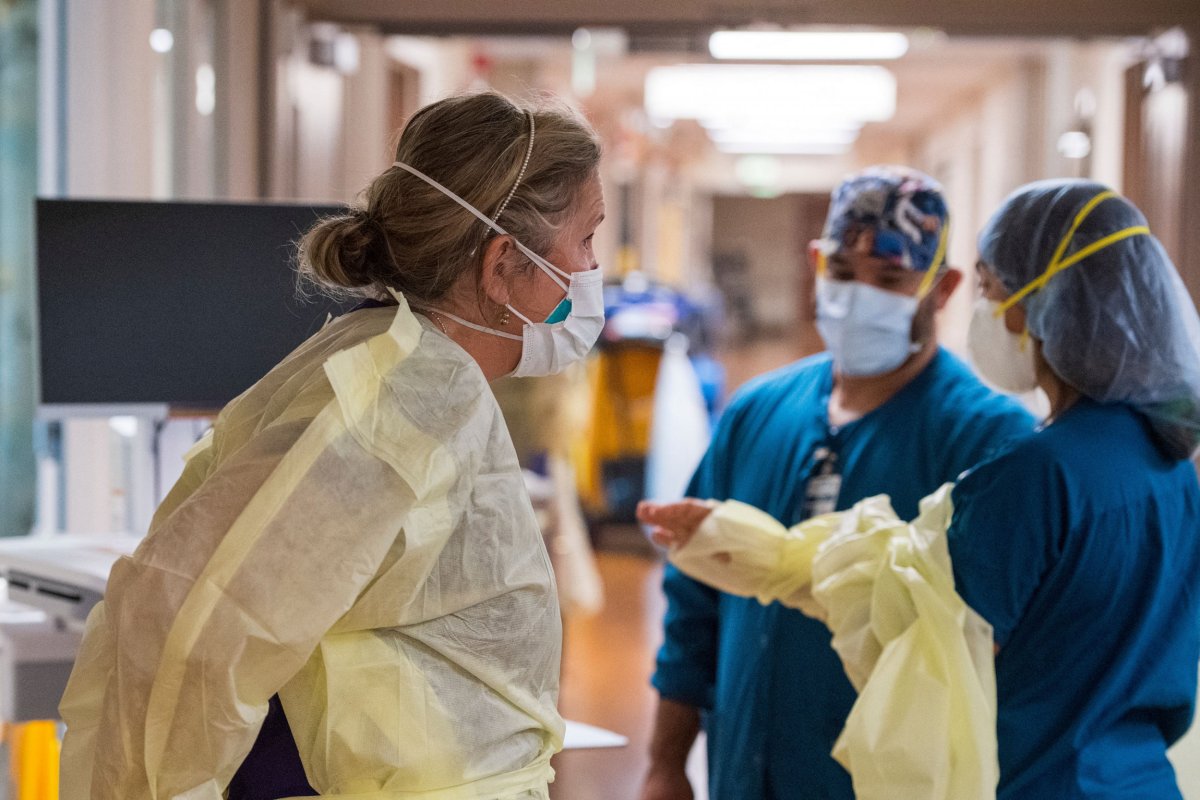
In other pandemic news, tumbling coronavirus case counts have some schools around the U.S. considering relaxing their mask rules, but deaths nationally have been ticking up over the past few weeks, some rural hospitals are showing signs of strain, and cold weather is setting in.
The number of new cases nationally has been plummeting since the Delta surge peaked in mid-September. The U.S. is averaging about 73,000 new cases per day, less than half of the nearly 173,000 recorded on September 13. And the number of Americans in the hospital with COVID-19 has plummeted by about half to around 47,000 since early September.
In Florida, Miami-Dade County's mask mandate could be loosened by the end of October if the encouraging numbers continue. A high school outside Boston became the first in Massachusetts to make masks optional after it hit a state vaccination threshold. With about 95 percent of eligible people at Hopkinton High inoculated, school leaders voted to allow vaccinated students and staff to go maskless for a three-week trial period starting November 1.
Still, there are some troubling indicators, including the onset of cold weather, which sends people indoors, where the virus can more easily spread.
With required mask use reduced in much of the U.S., the University of Washington's influential coronavirus forecasting model is predicting increasing infections and hospitalizations in November.
Also, COVID-19 deaths per day have begun to creep back up again after a decline that started in late September. Deaths are running at about 1,700 per day, up from close to 1,500 two weeks ago.
In sparsely populated Wyoming, which has one of the nation's lowest vaccination rates, hospitals are coping with more patients than at any other point in the pandemic.
"It's like a war zone," public health officer Dr. Mark Dowell told a county health board about the situation at Wyoming Medical Center, the Casper Star Tribune reported. "The ICU is overrun."
The vast majority of hospitalized patients in Wyoming haven't gotten a vaccine; the state's vaccination rate is only about 43 percent. Only West Virginia ranks lower.
During a three-week stretch this month, rural hospitals in Minnesota were caring for more COVID-19 patients than those in the state's major urban center, Minneapolis-St. Paul.
The strain on hospitals in Colorado forced a second county to reinstitute an indoor mask mandate last week, the Denver Post reported. Nearly 80 percent of COVID-19 patients in Colorado hospitals are unvaccinated.

Uncommon Knowledge
Newsweek is committed to challenging conventional wisdom and finding connections in the search for common ground.
Newsweek is committed to challenging conventional wisdom and finding connections in the search for common ground.
About the writer
Zoe Strozewski is a Newsweek reporter based in New Jersey. Her focus is reporting on U.S. and global politics. Zoe ... Read more
To read how Newsweek uses AI as a newsroom tool, Click here.








